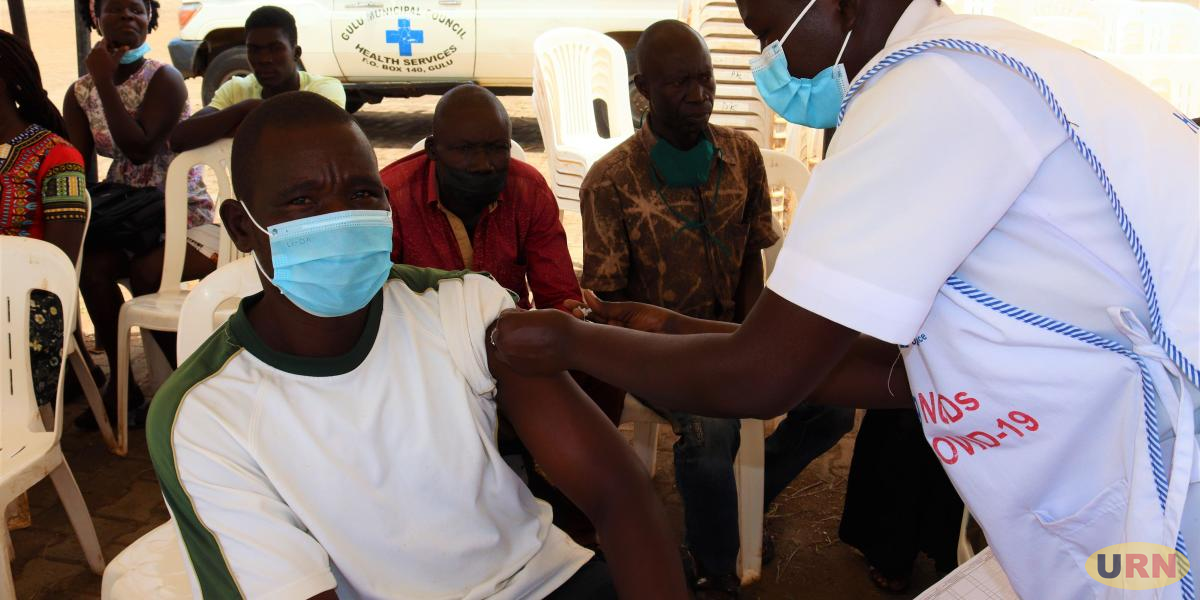
A litany of issues preventing people in low and middle-income countries from accessing COVID-19 vaccines, tests, and treatments have been misrepresented as vaccine hesitancy, according to new report from Matahari Global Solutions, the People’s Vaccine Alliance, and the International Treatment Preparedness Coalition (ITPC).
Researchers studying communities in fourteen low and middle income countries and territories found that a combination of undersupply of vaccines and treatments, underfunding of health systems, undervaluing of health workers, and poor adaptation to local needs were the key drivers behind low vaccination rates.
“Throughout this pandemic, low vaccination rates in lower-income countries have been conveniently dismissed as the result of ‘vaccine hesitancy’. Our report finds this allegation to be false. People face a litany of barriers to accessing COVID-19 vaccines and treatments – from undersupply of vaccines and treatments, to underfunding of health systems, and poor adaptation to local needs. These are issues of equity,” said Dr Fifa A Rahman, Principal Consultant, Matahari Global Solutions.
Leading global health researchers studied access to COVID-19 tools across Bangladesh, Democratic Republic of the Congo, Haiti, Jamaica, Liberia, Madagascar, Nepal, Nigeria, Perú, Senegal, Somalia, Somaliland, Uganda, and Ukraine.
Failing to meet WHO vaccination targets led to 600,000 preventable COVID-19 deaths from 8 December 2020 to 8 December 2021, equivalent to one death every minute. Oxfam and People’s Vaccine Alliance analysis of a study published in The Lancet: https://www.oxfam.org/
The report contradicts the repeated allegations from pharmaceutical companies and wealthy country leaders that people in lower-income countries are “vaccine hesitant”; an accusation again levelled by Pfizer CEO Albert Bourla at a recent public event.
The People’s Vaccine Alliance, a global coalition of civil society organisations campaigning for equitable access to COVID-19 vaccines, tests and treatments, described the report as evidence of “systemic racism” in the global coronavirus response.
“This report shows that communities have repeatedly been let down by a system geared towards protecting people in wealthy countries. People in the global south have been abandoned. Their lives have been treated as an afterthought. Local populations are expected to shoulder blame and be grateful for what vaccines they do receive, when there has been little effort to meet their needs. It is yet more evidence of the systemic racism that has plagued the global response to COVID-19,” Maaza Seyoum, Global South Convenor of the People’s Vaccine Alliance.
“Governments, pharmaceutical companies (including domestic manufacturers) and international agencies must meaningfully address the real issues that prevent people from accessing vaccines and treatments,” said Nadia Rafif, ITPC Advocacy and Influence lead.
Investing in more pharmaceutical manufacturing in lower-income countries and maximizing the use of the existing public health safeguards such as the TRIPS flexibilities, could improve reliability of access to vaccines and treatments. It could also go some way to countering the distrust of Western medical products that exists in some parts due to phama greed, health nationalism, and a legacy of colonial oppression and racist medical experiments.”
The report found that:
- Testing and vaccination sites have been inaccessible, meaning true infection and death rates are likely to be far higher than official figures. PCR tests results can take anywhere from 8-12 hours in Bangladesh to more than two weeks in rural DRC. People cannot leave work at short notice, travel long distances to a vaccination/testing site, and then wait for a long unpredictable period of time. For rural populations and nomadic people in countries like Somalia, this problem is particularly acute. Mobile vaccination and testing is not widespread enough.
- Vaccine supply is still a major problem. Vaccines have been delivered inconsistently and in insufficient numbers, leading to stock fluctuations at vaccination sites. Doses can arrive with little or no notice or information about what kind of vaccine will be delivered or whether they are suitable to conditions in a country. Dr Saeed Mohamood from Somaliland’s Ministry of Health said, “Sometimes we will find out that the Somaliland shipment is on a plane in the air, en route, and we do not know when it’s going to expire and how much resources we will have.”
- Access to antiviral treatments is nonexistent in most countries surveyed. Health Workers on the ground in some countries are not even aware that treatments like Paxlovid exist. Some countries will have access to doses through generics licensing agreements, but that is unlikely to happen this year, meaning the grave inequities experienced with the global vaccine rollout will be repeated with treatments. Peru, among other middle-income countries, is considering overriding patents to secure access.
- People cannot access accurate information in a format that is accessible to them, reducing the likelihood of vaccine uptake. Information campaigns are often in the “official language” of former colonisers (e.g. English, French, Spanish), instead of local languages, and use technical terms that are hard to understand. Richard Musisi, Executive Director of MADIPHA in Uganda, said: “When the key vaccinations started, the fact [was] that people could not find access to such information, most of the information was communicated in English, it was not put into local languages”
- A history of colonial oppression and racist medical experimentation mean that people in some areas distrust Western medical products delivered by white doctors and Western aid programs. This has compounded with access issues and a broader distrust in government in certain areas. Building more pharmaceutical manufacturing in lower-income countries could help tackle these perceptions, campaigners say..
- Oxygen supply planning and financing has been poor. A public health officer at WHO Nigeria told researchers “The Oxygen plant breaks down whenever there’s high demand and it needs upgrading in other wards and further installation of another one with regular maintenance.” Governments need multiyear oxygen supply and infrastructure plans that include national inventories on oxygen infrastructure and technical support, and modified donor requirements that include medical oxygen.
- Essential community health workers often go unpaid. Vuyiseka Dubula, former head of the Treatment Action Campaign, described the erratic and sometimes non-existent payment as “a form of modern day slavery”. In DRC, nurses in North Kivu earn just US$80 per month, and some reported not having been paid since the beginning of the pandemic. A clinician in Haiti, Dr Marie Delcarme Petit-Homme, told researchers “Sometimes doctors and nurses can go 6 months, a year without receiving remuneration. Lower bands have it worse, they don’t really have access to remuneration. Sometimes we are forced to leave the country if we want a better pay.”
Ends