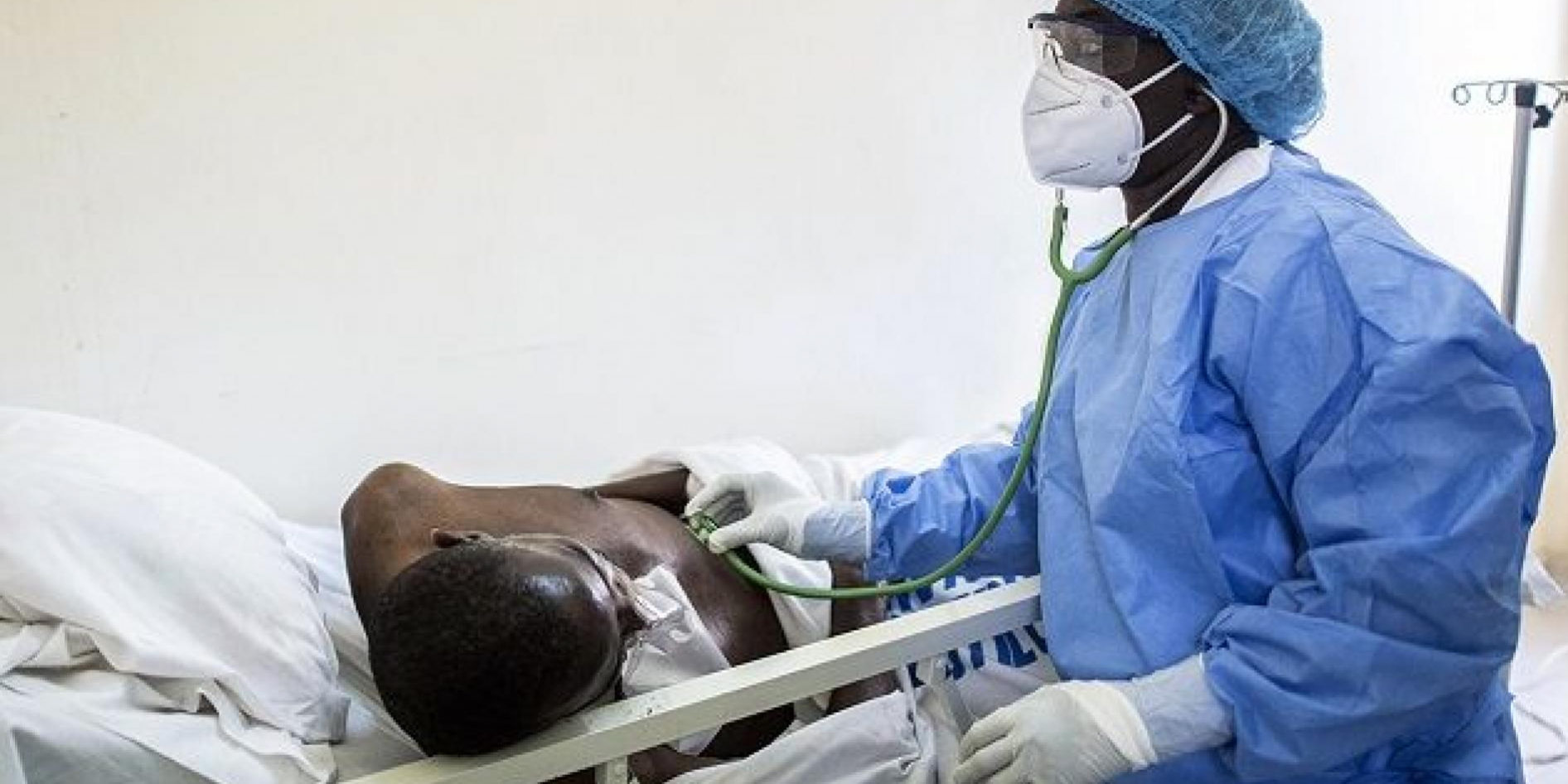
On May 28, 2021, Irene Nakasiita, the head of communications and Public Relations at the Uganda RedCross Society tested positive for COVID-19. She was admitted to Jinja Regional Referral Hospital on the same day since she had difficulty breathing.
Nakasiita describes her stay at the hospital as horrible with doctors relegating their duties to nurses who have limited knowledge in handling complicated cases of COVID-19.
According to Nakasiita, due to the lack of staff, the health workers advised her to get a caregiver from home to look after her after she was weaned off from oxygen. COVID-19 treatment protocols do not allow family members to cater for the sick due to the highly infectious nature of the disease.
In addition to lack of staff, Nakasita says the hospital did not provide them with the meals associated with COVID-19 hospital management. She says she had to pay someone outside the hospital to provide her with food. Nakasiita is not alone.
According to the administrators in some regional referral hospitals in the country, many share Nakasita’s experience due to lack of human resource. Dr. Paska Apiyo, the head of the COVID-19 treatment unit at Gulu Regional Referral hospital, says that many of health workers in ICU do not want to work.
“We have very few committed staff to support the patients in the COVID-19 Treatment Unit-CTU and this is serious since we need staff to look after the patients. Many of the patients admitted now need round the clock care,” Apiyo said.
Dr. Florence Tugumisirize, the Director of Jinja Regional Referral Hospital told URN the hospital can no longer afford to care for patients as they did in the first wave.
Tugumisirize says they are facing human resource challenges because many health workers do not want to attend to COVID-19 patients while families have stopped others from working in Covid-19 Treatment Units.
At least 32 COVID-19 patients have died in the Intensive Care Unit of Jinja Regional Referral Hospital over the last two months. The death occurred between April 13, 2021, and June 13th, 2021 during the second wave of COVID-19. The same unit handled 324 patients between March 2020 and February, 2021 in the first wave.
Thirty of the 324 patients didn’t make it, five were referred to Mulago National Referral Hospital while 281 were successfully treated and discharged after full recovery. The hospital has so far admitted 156 COVID-19 patients in the second wave. 124 of these were treated and discharged while 32 succumbed to the virus.
Tugumisirize said their ICU has 32 beds but they currently have 53 patients. She says that due to the increasing number of COVID-19 patients and referrals from other facilities, they have been forced to expand the ICU by temporarily converting the general male ward and part of the private wing into COVID-19 treatment wards.
She however says that despite the current boost, which has raised their daily oxygen output capacity to 70 oxygen cylinders, the demand is increasing each day.
Intern doctors in charge
With shortage of staff many hospitals are relying on the intern doctors and nurses without the required training or expertise in most cases to handle infectious diseases.
“Before we had many doctors working but now, we only have a team of five which comprises of three nurses and doctors that work in shifts. Most people from other wards that worked with us in the first wave refused to join us. So we accept the little help that we get,” Apiyo said.
Dr. Mkukuzi Muhereza, the secretary-general of Uganda Medical Association, an umbrella body for all health workers, says that while doctors promise to provide care to patients in the Hippocratic Oath, they are right in refusing to expose themselves to COVID-19.
He says if the government cannot provide all health workers with enough Personal Protection Equipment-PPEs, health workers have to protect their lives first even if this means not showing up for work.
According to the UMA, the doctor’s hesitancy to work on the COVID-19 ward is attributed to the lack of PPE, delayed payment of allowance and salaries. In addition to this, Apiyo says that some doctors do not even get drinking water.
“Before the doctors would be given a food allowance that would encourage them but that is no longer there. The doctors have no morale to work. They are not even given drinking water,” she adds.
Officials from the ministry of health that URN spoke to about the dilemma of patients said they were not aware of the problem. Dr Charles Olaro, the Director of Health Services promised to look into the matter.
“We had not yet heard about this happening but we shall look into it and see what exactly is happening,” Olaro said.